In Chelsea Mazur’s dreams, she’s trying to use her inhaler but it’s not working.
The 30-something Winnipegger was diagnosed with asthma as a child. For years, she has kept it under control. But last summer’s wildfires and heat wave in Manitoba, which choked the skies with toxic, heavy smoke for weeks, presented a dilemma.
To cool off her scorching apartment, Mazur had to run her air conditioner. This pulled in smoky air, which triggered her asthma and forced her to use her inhaler.
She began refilling her prescription more often, worried she might run out, and checking the air quality index daily before leaving her home. The anxiety and stress of her hypervigilance invaded her sleep.
“I’d have a dream where I’m having trouble breathing,” she said in an interview with The Narwhal. In her dream, she reaches for her inhaler, but it doesn’t function. Then she wakes up. “There was more of that last summer,” she said.

Mazur, who works as a digital content specialist at the University of Manitoba, said she knows wildfires are becoming more frequent and more intense due to climate change, which is being driven by carbon pollution from fossil fuel use. She considers herself lucky she can access medicine for her asthma, but fears what the future may hold as the planet continues to heat up.
“It makes me worry about when I’m older, in my 60s and 70s. What’s it going to be like then to have asthma?” she said. “What’s the air quality going to be like, and how is it going to affect me?”
More than five million Canadians, like Mazur, live with respiratory conditions. As climate change makes wildfire seasons worse, many of them pay the price with their lungs.

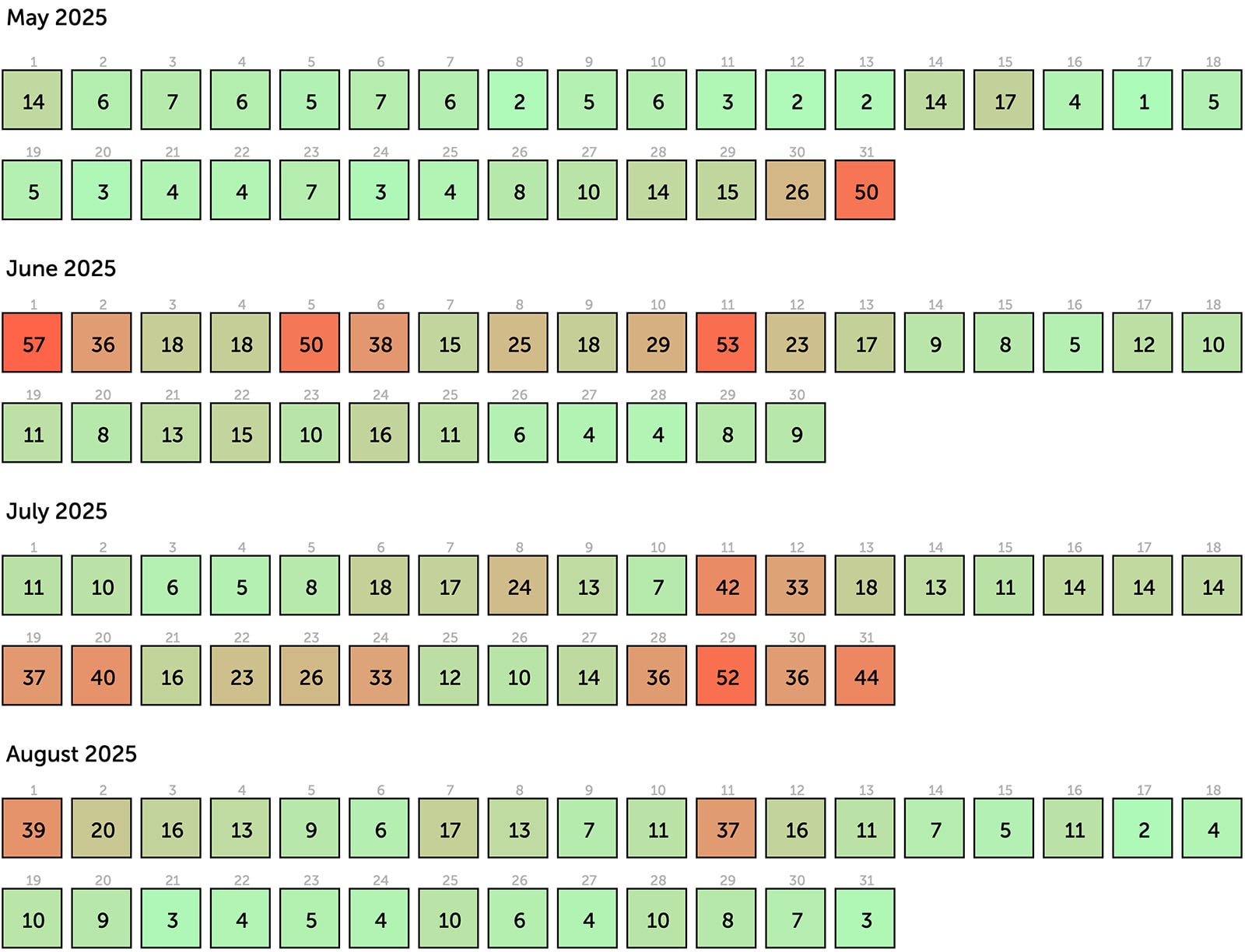
Smoke days were responsible for up to a 23.6 per cent increase in asthma-related hospital emergency visits in Ontario in 2023, according to research published in the Canadian Medical Association Journal. Almost all respondents to a 2025 Asthma Canada survey reported worsening asthma symptoms with poor air quality, and most also reported a decline in their mental health.
Smoke from wildfires is a form of air pollution, carrying toxic gases like sulphur dioxide, nitrogen dioxide and carbon monoxide, as well as fine particulate matter. Other sources of air pollution, from car and truck exhaust to power plants and oil and gas facilities, are also hazardous to our health.

Air pollution can cause heart disease, strokes, chronic lung diseases and cancer, the World Health Organization notes. Federal research has found it contributes to about 17,400 premature deaths each year in Canada. In B.C., a nine-year-old died in 2023 after an asthma attack was made worse by wildfire smoke.
And that’s just one health impact of pollution and extreme weather. People exposed to air pollution also have a higher risk of developing Alzheimer’s disease, according to a study in the journal PLOS Medicine. Doctors and counsellors across Canada note that conditions from poor mental health to Lyme disease to detached retinas can be linked to the effects of a warming world.
When Canadians talk about affordability, the discussion often revolves around the cost of fuel. While we pay for gasoline and diesel with our credit cards, in study after study, scientists have shown we also pay with our bodies.
In broad terms, it’s possible to juxtapose the economic output of fossil fuels with health costs. The federal energy regulator, for example, has reported the total value of crude oil exports from Canada was $138 billion in 2024. A Health Canada report that same year found the total cost of health impacts attributable to air pollution in 2018 was $146 billion.
But in other ways, it’s tough to quantify how much fossil fuels and climate change are costing Canadians and our health-care systems.
There’s a perpetual ripple effect of consequences that often go unaccounted for, Ottawa physician Helen Hsu said. Hsu specializes in addiction and mental health and is a spokesperson for the Canadian Association of Physicians for the Environment.
The indirect costs of climate change show up in things like premature deaths, she said, or the number of days people are sick and can’t work — which also brings a financial cost for businesses, though she’d rather not focus on that.
“It feels a bit ghoulish to say, ‘Well, how much do you contribute to our economy?’ ” Hsu said.
“I think certainly we do pay with our bodies, and we need to start really thinking about that.”

This is part of Who Pays?, a series at The Narwhal looking at the intersection of the environment and the economy
Alex Goatcher paid for B.C.’s 2021 heat dome and wildfires in terms of both physical and mental health, he told The Narwhal in an interview. That year a high-pressure system trapped heat on the ground, like an oven. It led to 619 deaths. Scientists have connected the severity of the wildfires and heat during this time to climate change.
Goatcher is a visitor services worker for Parks Canada and was living in Field, B.C., and working at Yoho National Park when the heat and fires trapped him inside for weeks.
He said he loves hiking on his days off, but couldn’t venture outside due to his asthma. Air conditioners were uncommon in the area until recently, he said, so he didn’t have one at the time.
“Being stuck inside during the prime of summer, with it being scorching hot and the smoke, it really negatively affected my mental health, to the point that I noticed my interactions with my neighbours were more hostile,” Goatcher said.

Adding to Goatcher’s frustration was the way his asthma disrupted not just his immediate work, but his long-term career prospects. His supervisor, concerned for his health, ended up grounding Goatcher during the heat dome when other staff were sent out. He was also forced to turn down an internal job opportunity because it would have involved working outdoors.
“It never crossed my mind about the smoke and the fires and all that,” he said. “I never thought that this would be any sort of thing I’d have to really deal with.”
Métis sociologist Trisha McOrmond is on the national council of the volunteer climate action network For Our Kids. She uses her training in trauma-informed coaching when broaching the topic of climate change with people who are more vulnerable to extreme weather, including those who work outdoors in jobs like construction or farming.

“There is a level of frustration, and almost like a compartmentalization,” she said — a defence mechanism people use to avoid confronting the stress of knowing they will have to deal with more climate-change consequences at their job. “It’s hard for them to open up and have those conversations, because they have to put it away.”
She said it’s a challenge to put a specific dollar figure on the mental-health impacts of evacuations or other climate-related personal emergencies, because they can appear years after specific events and seem disconnected.
“They’re not showing up by people saying, ‘Oh, I’m worried about climate change.’ It’s showing up as disengagement at work, it’s showing up as [fatigue and burnout]. It’s showing up as increased domestic violence and interpersonal violence,” McOrmond said.
“We don’t see the cost directly, because we don’t have a system that measures those costs. And since we don’t measure them, we don’t see them.”
Most Canadians have come to understand how some unhealthy behaviours are connected to their health — like how smoking cigarettes increases their risk of lung cancer. But many still don’t see the associations between fossil fuel use, climate change and health impacts, Doris Grinspun, the chief executive officer of the Registered Nurses’ Association of Ontario, said in an interview.
This is especially true for work days lost to climate-linked health problems, Grinspun said.
“I don’t think people really are connecting the dots,” she said.
“When more pipelines get built, or we will not put an end to fossil fuels, we don’t say what the consequences will be, in human life, in disease, in death and in debt. We are already paying for it.”
Those costs manifest in ways we may not recognize — like our vision.
Particulate matter, certain gases and other pollutants hurt our eyes as well as our lungs, Montreal ophthalmologist Marie-Claude Robert said. Research has connected higher levels of particulate matter and nitrogen dioxide with more hospital emergency department visits for conjunctivitis, or pink eye.
Other research has suggested a link between heat waves and an increased risk of retinal detachment, which can cause flashes of light and dark spots in vision, as well as blindness if left untreated.
“In my personal practice, when we had heavy smog in Montreal from wildfires out west or up north, a lot of our patients would come in with acute worsening of their symptoms from that poor air quality,” Robert, who represents the Canadian Ophthalmological Society, said.

There are a limited amount of treatments for these symptoms, and each one comes with costs. High-quality artificial tears, for example, can cost up to $30 a bottle and are usually not covered by insurance, she said.
Climate change is also increasing the risk of Lyme disease, as ticks spread into more locations and last longer each season. That disease can lead to chronic disabilities that can remove someone from the workforce, Hsu, the Ottawa physician, said. She’s personally seen a middle-aged man with no pre-existing medical conditions who contracted a tick-borne illness and became paralyzed for months.
Hidden costs also fall disproportionately on vulnerable populations like children, the elderly, those with pre-existing disabilities and pregnant women, Hsu said.
Heat can trigger premature labour, and keeping preterm babies alive is very expensive for the health-care system. It’s also emotionally and financially difficult for parents — premature birth is the leading cause of mortality in infants in Canada, and those that survive can have lifelong respiratory issues.
Climate change-related health costs also show up for those who live in remote regions, including First Nations who have to be evacuated from wildfires in their territories, and Inuit whose lands are warming faster than the rest of the world.
And the financially vulnerable are least able to afford measures to protect themselves, like air conditioners or air purifiers.
Hsu said one of her patients is paralyzed from the neck down and can’t afford air conditioning. During heat waves, he often passes out.
“He’s just living in a state of suffering every summer, and it’s incredibly unfair. It’s wrong that we’re asking those who are most vulnerable in our society to pay that cost,” she said.

For Melanie Hoffman, a school board trustee and community organizer from Edmonton, the emotional toll and financial costs of climate change are front and centre.
As an infant, Hoffman’s now eight-year-old daughter contracted a virus that infects the respiratory tract and had to be hospitalized, eventually requiring airway reconstruction surgery, she said. As a result, she pays close attention to air quality.
A few summers ago, when the city was engulfed in wildfire smoke, Hoffman realized her daughter’s outdoor-focused camp didn’t have guidelines in place for how to accommodate smoke days by bringing the kids inside.
“I felt really concerned for my daughter’s health, but also for the youth that were running the camp. This was their summer job, and they were required to be outside. They weren’t given the tools to manage that,” she said.
She and her husband had to solve the logistical problem of who could take time off work to keep their daughter home. She understands that this is a privilege.
“If your kids need you home, if you’re self employed, you’re going to pay for that in lost revenue. And if you don’t have benefits from your employer, you’re going to pay in lost days of work,” she said.

Just as difficult was navigating the tension between wanting her to be able to go to the camp and the uncertainty about exactly how harmful the long-term consequences of exposure can be.
“I had not processed for myself the fact that these are the rest of the summers of my daughter’s life. Growing up, certainly in her youth, she is not going to know a summer that isn’t in a changing climate,” she said.
Hoffman holds a PhD in chemistry, is the former program manager for Capital Region EcoSchools with the Alberta Council for Environmental Education and volunteers with the Climate Reality Project Canada. She knows science-based climate solutions, like transitioning to renewable energy sources, using heat pumps and improving public transit, work. But, she said, there’s “an issue of political will and cultural inertia.”
McOrmond, the sociologist, sees a glimmer of hope in the course she teaches on systems thinking, a way of examining the different components of why the world is set up the way it is and how decisions are made as a result. She says students bring excitement and enthusiasm to conversations “as they start to realize that there is another way of looking at this world that isn’t just about extraction.”
Some of the climate solutions related to health she points to are movements to source local ingredients and share food, community-supported agriculture in rural areas to help farmers get food to local markets, local community festivals, volunteer-run shops and food banks.
“We have to stop looking at the big things that are scaring us, and start looking at the small things that are saving us,” she said.
“The more local we are, the safer we are. I know that sounds contradictory, but once we’re safe locally, we can begin to make changes and we can move the needle on a bigger scale. We just have to know each other, and have to trust each other.”
— With files from Julia-Simone Rutgers
Updated on April 23, 2026, at 12:20 p.m. ET: This story has been corrected to note that Melanie Hoffman is the former, not current, program manager for Capital Region EcoSchools with the Alberta Council for Environmental Education.