In early December 2021, a grisly scene unfolded along Manitoba’s western border: marksmen armed with semi-automatic rifles loaded into a helicopter and hovered low over the prairie.
There was a burst of gunfire. A deer racing across the open field collapsed, caught by the marksmen’s bullets. A cull was underway.
The marksmen, hired by Manitoba’s department of natural resources, had been tasked with slaughtering local deer in an effort to contain the spread of the deadly so-called “zombie deer” disease.
Residents on both sides of the Manitoba-Saskatchewan border watched in horror as marksmen in the air and on the ground picked off more than 500 deer over the course of the four day cull, airlifting the carcasses away. Video of the cull began to circulate on social media, as some residents decried the “nauseating” conservation tactics.
“It’s just disheartening to see,” Saskatchewan resident Richard Geres told the Winnipeg Free Press at the time. “It’s not what conservation stands for.”

Chronic wasting disease, as “zombie deer” disease is more commonly known, had at last breached the Manitoba border, prompting the province to dust off an emergency response plan 20 years in the waiting. The progressive neurological disease — which affects cervids including deer, moose, elk and caribou — is contagious, incurable and fatal. The Manitoba government has identified a total seven positive cases since 2021, including two more last week.
Though many witnesses to the cull found the tactic alarming, experts say Manitoba’s swift actions may be the only way to stop the rapidly spreading disease in its tracks.
Left unchecked, chronic wasting disease is likely to devastate cervid populations and wreak havoc on ecological systems. Biologists also worry that it could one day infect humans, something some experts fear could spell catastrophe. As Alliance for Public Wildlife director Darrel Rowledge puts it, “it is the ultimate nightmare disease.”
Since its discovery in captive deer at a Colorado research facility in the 1960s, jurisdictions across North America have been working on strategies to control, monitor and mitigate it. The disease has spread rapidly — often thanks to human activity — and today is found in farmed and wild cervid populations in four Canadian provinces and 30 American states and around the world, from South Korea to Norway.
Learning from jurisdictions already afflicted by uncontrolled spread, Manitoba saw last year’s cull as an opportunity to take an aggressive approach and hold the disease at bay.
“You’ve got to make a decision on whether you respond or whether you step back,” Manitoba wildlife health biologist Richard Davis says. “Every jurisdiction that’s tried to step back … that’s never worked.”
What is chronic wasting disease?
Chronic wasting disease is part of a family of diseases caused not by a bacteria, virus or fungus, but by misfolded proteins, called prions. Normally, an animal’s body produces strings of proteins that fold into specific shapes to perform specific functions; a prion occurs when those folds — for reasons health professionals don’t yet understand — go awry.
Prion diseases cause a type of infection called “transmissible spongiform encephalopathies” — a type of contagious disease that creates sponge-like holes in an animal’s brain.
Chronic wasting disease isn’t the first prion disease: scrapie has been around in sheep populations for more than 200 years and bovine spongiform encephalopathy made a global splash when an outbreak of so-called “mad cow disease” struck the United Kingdom in the 1980s. Mad cow disease was particularly nefarious, and more than 200 people eventually died of a related brain disease caused by eating infected beef.
These neurological diseases progress slowly and it can take several years for symptoms to appear. It’s those end-stage symptoms that earned chronic wasting disease the “zombie deer” description: infected animals stumble, drool and appear listless and emaciated, making them far more likely to be killed by hunters or vehicles than healthy animals.

But unlike mad cow disease, which both cows and people can get from eating infected feed or meat, chronic wasting disease is highly contagious among cervids. The infection passes between animals through fluids — saliva, urine, even placenta — but it’s also known to persist in the environment for a long time. Infected carcasses create “supersites” where prions leak into the soil. They can be taken up into the roots, leaves and stems of plants, they can persist in water and they stick to minerals in clay-based soils, which describes much of Manitoba, where they can become up to 680 times more infectious.
Prions also can’t be wiped out by any known disinfectant, sewer treatment, alcohol or formaldehyde. The only nearly successful attempt to eliminate the infectious particles involved burning them at nearly 600 C — the melting point of aluminum.
So far, no cases of chronic wasting disease have been found in humans. But while experts believe the risk is low, it’s not zero. Much has been written about the disease’s potential to one day jump the species barrier; a 2020 Health Canada advisory noted the risk of human transmission is still “theoretical,” but recommended taking a “precautionary approach” in light of more recent “conflicting evidence.”
Zoonotic diseases — which pass from animals to humans — are responsible for a host of commonly known illnesses like measles (which originated in cattle), AIDS (from hunted chimpanzees), SARS (from palm civets) and the recent COVID-19 pandemic (thought to have jumped from bats to pangolins to people). It’s estimated that between 60 and 75 per cent of “new” human pathogens come from the animals that humans butcher, process and eat.
That figure only stands to rise as people disrupt natural ecological systems through development, resource extraction and trade. These activities, which push people and wildlife closer and closer together, have led scientists to warn pandemics caused by zoonotic diseases are becoming all the more likely.
In the case of chronic wasting disease, scientists have yet to reach consensus about the risk of human transfer. Experts are still researching whether humans could eventually contract and spread the disease through direct contact with fluids or eating infected meat, but warn even “a single case could create a crisis.”
‘Gross dissection lab’ on front lines of monitoring
Such potential catastrophe was top of mind for biologist Davis last fall when the first signs of chronic wasting disease came through his laboratory door.
On Oct. 14, 2021, Manitoba’s wildlife health surveillance team found an “unhealthy” mule deer buck near Dropmore, Man., a small town just a stone’s throw from the Saskatchewan border. Suspecting brainworms, conservation officers euthanized the deer, then drove the carcass 150 kilometres east to a non-descript row of sheds on the outskirts of Dauphin, Man. The deer would later test positive for chronic wasting disease, marking the province’s first case in more than two decades of sampling, testing and surveillance.

Those sheds are home to the province’s lone wildlife health laboratory, where Davis has spent 16 years leading a host of disease management programs. “It’s basically a gross dissection lab,” Davis says during a recent tour.
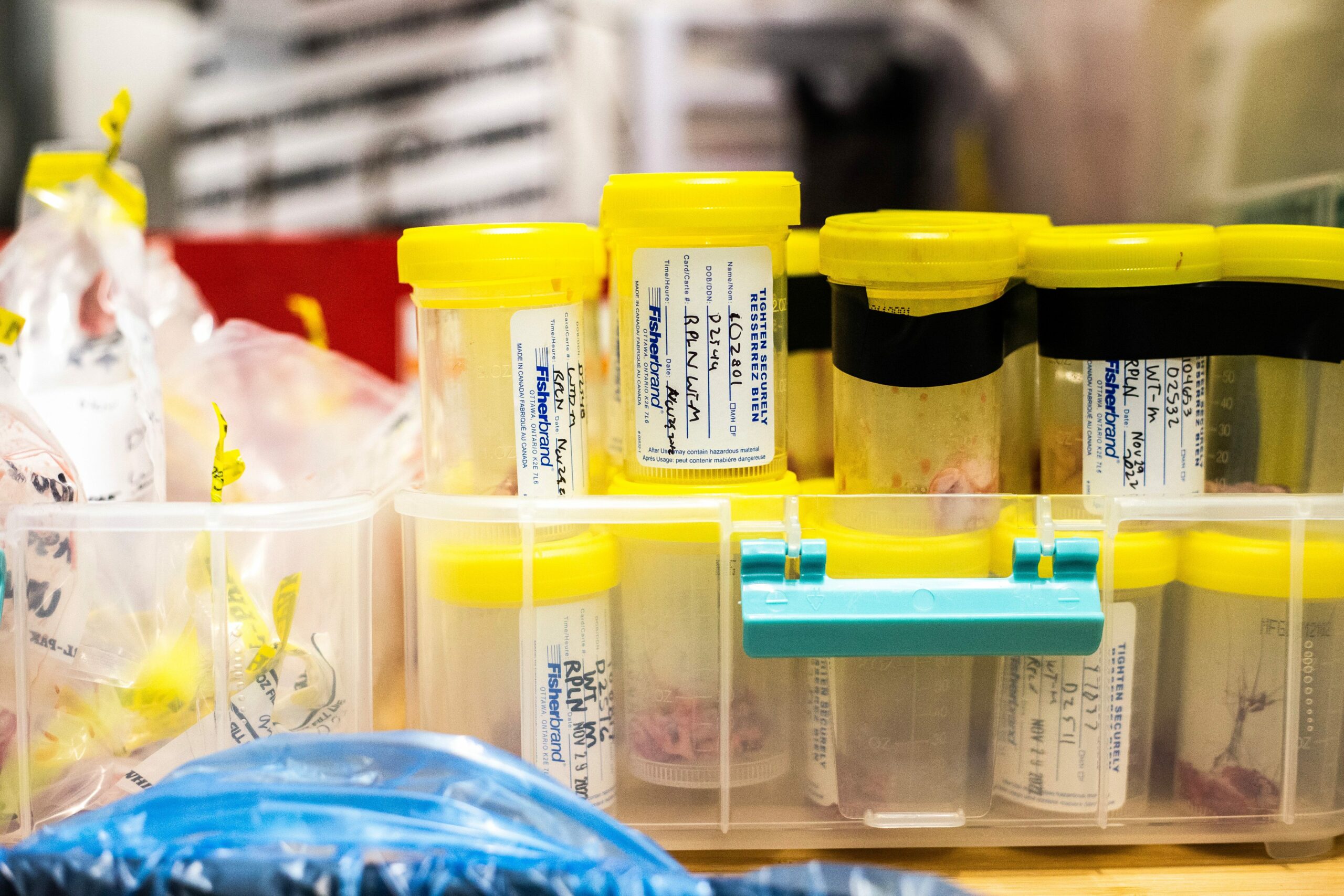
In two crowded rooms, a crew of about 10 decked out in rubber boots, blood-spattered aprons and elbow-length gloves work through piles of bagged animal heads. A string of connected garages house even more heads: when the sheds ran out of room, the team started storing them in the back of a semi-truck during the winter, trusting below-zero temperatures to keep the heads frozen. Staff work in pairs: one person records notes while another wields the knife, slicing out tissue samples to send away to a federal lab in Ottawa for testing.

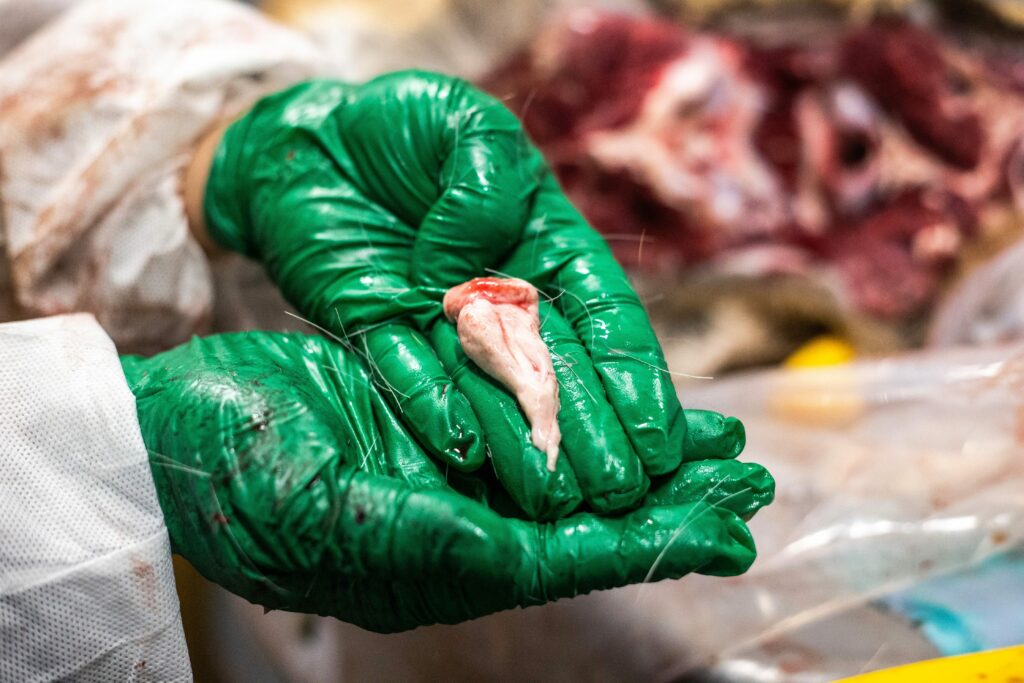
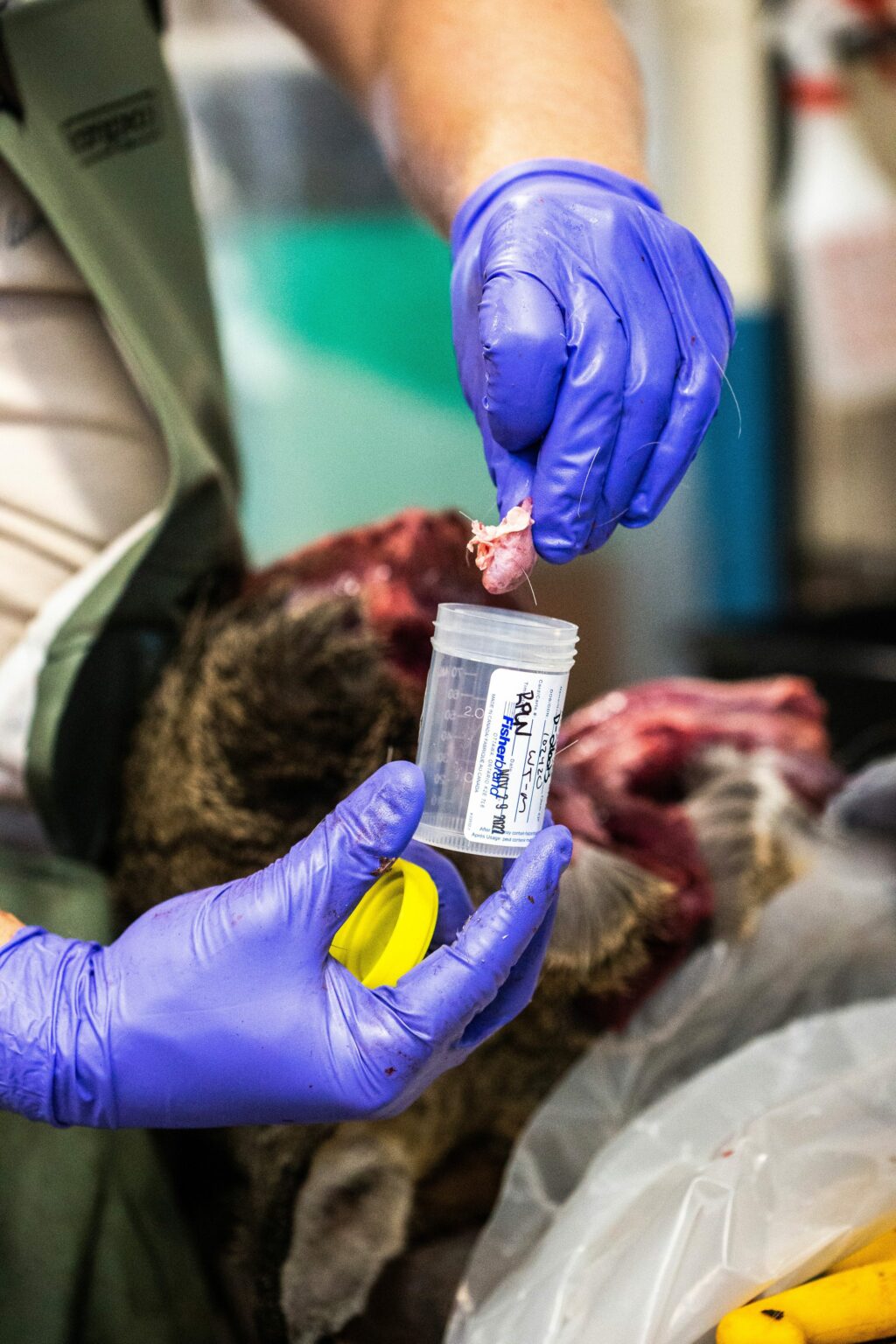
Sampling for chronic wasting disease involves cutting out either the two small, bean-shaped lumps just under the animal’s jaw near the windpipe, called medial retropharyngeal lymph nodes, or the obex, a small fold of white matter where the brain meets the spinal cord. Each person can sample anywhere from 20 to 60 heads a day, so the lab processes hundreds of samples every shift, but this year they’re struggling to wade through the backlog.
Part of the problem is that the testing process is slow, Davis says. The federal lab receives samples from several provinces — including Saskatchewan and Alberta, where the disease is widespread — so results can take up to 12 weeks.
“Everything is bottlenecked,” Davis explains. “There’s no accredited lab in Manitoba to do testing, so we’re limited by that.”
This year’s backlog is unique. Before the first cases were found in 2021, only hunters who shot deer along the western border were required to drop off the animals’ heads at designated freezers scattered around the province. Testing elsewhere was voluntary. Typically, the lab processed an average of 500 animals per year. In 2021, the lab sent about 1,600 samples out for testing, the majority of which were hunted. This year, Davis expects the team will sample more than 4,000 heads — hence the pileup.
When the Dropmore deer tested positive, the province’s plan of attack changed. Cervid hunting closed temporarily in the region, then reopened with a specific edict to hunt white-tailed and mule deer. Area hunters harvested 132 deer in the fall of 2021, all of which were brought in for testing.
“It sounds as if we’re being Draconian, forcing hunters to give up their trophy,” Davis says. “But it’s not to make it onerous for the hunter, it’s because it’s so important to get every possible sample we can.”
By mid-December last year, three more deer had tested positive, prompting the province to escalate containment efforts.
‘Aggressive’ strategies needed to contain chronic wasting disease
When chronic wasting disease landed in Saskatchewan in 1996, foremost expert Elizabeth Williams — a veterinary scientist credited with first classifying the disease — was asked what Canada should do if the disease spilled over into wildlife.
“You’ll have to be aggressive; remove all sources and all potential movement,” she said.
“Cut wider and deeper than you ever think necessary. The deer will come back; but you’ll get one chance. If [chronic wasting disease] gets widely established, you’ll have it for a very long time.”
It’s that advice Manitoba aimed to follow when they launched the cull.
“We absolutely hated it,” Davis says. “Nobody in their right mind wants to go and do that.”

But fearing further spread, the province harvested more than 500 deer in a 10-kilometre radius around the positive tests. Davis explains the plan, at first, was to “drop a pin on the map [and] draw a circle 20 kilometers around it” — roughly the winter home range of cervids – and “eradicate” all the cervids within it.
“But that wasn’t really socially acceptable,” he notes.
Critics mounted several arguments against the cull: the disease doesn’t impact people and infected deer can live several years with the disease. In the end, Manitoba scaled back the radius and focused primarily on mule and white-tailed deer. Davis says he was disappointed by the less aggressive approach, but it wasn’t the only management strategy the province applied.
Manitoba nearly tripled the mandatory sampling area, which now includes hunting zones from Flin Flon, Man., all the way down the western border to the United States, then across the southern border to Ontario. It also introduced a new hunting permit for mule deer — previously considered a threatened species due to low populations in Manitoba, and banned for hunting except by Indigneous communities.
“We’ve worked for years trying to keep it across that artificial border,” Davis says. “Now it’s going to trickle in a little bit … but we’re working really hard to stop it from getting anywhere else in Manitoba.”

The province maintains there’s no evidence of spread beyond the cluster of positive cases near the Saskatchewan border. Davis says he’s “fairly confident” the disease hasn’t taken hold in the more common wild white-tailed deer, but mule deer have been a bit of a blind spot. Because of the long-standing hunting ban, mule deer were rarely submitted for testing, but male mule deer seem particularly susceptible to the disease — all of Manitoba’s positive cases have been in mule deer bucks so far. The low population numbers in Manitoba may be a saving grace, Davis explains. Chronic wasting disease passes quickly through deer families, but with most mule deer wandering over from Saskatchewan, Davis is holding out hope the disease hasn’t had much of a chance to spread.
Still, Davis admits the province’s sampling program has been “hit or miss” over the years. Though it had been spreading in the U.S. since the late 1960s, chronic wasting disease landed on the Prairies in 1996, when an infected elk from South Dakota was imported to a game farm in Saskatchewan.
Manitoba started monitoring in 1997, setting up voluntary sampling zones along its southern and western borders. But five years passed without a positive case, and a more pressing wildlife disease — bovine tuberculosis — was on the rise, so the chronic wasting disease program stalled.
Then Davis, who had been running the tuberculosis monitoring program since 2006, noticed Saskatchewan lapsing in their chronic wasting disease patrols along the shared border.
“Some of the management programs [Saskatchewan] put in place were, in hindsight, not the best,” Davis says. “They just weren’t doing it to our level of satisfaction.”
Saskatchewan’s early control programs were aimed at reducing mule deer numbers near positive tests, which were mostly found on game farms. After finding positive cases in the wild, Saskatchewan set up hunting incentive programs — such as an “earn a buck” system that allowed hunters to shoot mule deer bucks if they brought two mule deer doe heads in for voluntary testing — but shied away from more aggressive measures, such as mandatory testing or restricting game farms.

According to data from the Canadian Wildlife Health Cooperative, there were just shy of 500 positive cases in Saskatchewan spread out between 1997 and 2016. Though voluntary testing means numbers can fluctuate year over year, the disease is becoming more prevalent: last year, the province found 644 positive cases.
In the South Saskatchewan River valley that runs through the central part of the province, the government estimates approximately 87 per cent of male mule deer and 34 per cent of female mule deer have the disease — among the highest rates in the world. Yet testing remains voluntary in the province, and leaders are still debating strategies to limit further spread both in the wild and on game farms, according to an emailed statement from the Saskatchewan Ministry of Environment.
With the disease encroaching, Manitoba “got scared,”Davis says, and introduced more stringent surveillance measures.
Prevention key to mitigating chronic wasting disease spread
Containing and eradicating outbreaks is only one piece of the puzzle. Much more important, Davis says, are preventative measures, which focus on limiting human factors that increase the risk of spread.
It’s illegal to import an unprocessed deer carcass into Manitoba. The province also bans feeding deer and setting out bait, and only allows elk game farms.
Experts agree game farms are considered high risk for spreading disease quickly among closely congregated animals, while farmed animals shipped to other jurisdictions are a leading cause of artificial spread.
In 2019, the Saskatchewan Wildlife Federation called for an end to wild game farms, believing chronic wasting disease to be “widely concentrated” on the farms. At the time, just 15 per cent of the province’s nearly 200 game farms were enrolled in the Canadian Food Inspection Agency’s voluntary herd certification program, which allows farmers to sign onto a federally regulated disease management program and be certified disease-free.

Most Manitoba game farms that kept cervids captive for breeding, antler products, trophy hunting and occasionally meat production, were nixed in the early 2000s. A couple dozen elk farms still sell animals to trophy farms in the United States, and Manitoba’s largest elk farms have been part of federal disease monitoring for many years. Trevor Farmer, owner of the Stonewood Elk Ranch just north of Stonewall, Man., says his family farm has been monitoring for chronic wasting disease, tuberculosis and other wildlife illnesses since the early 2000s.
Farmer says it’s a “myth” farmed cervids are a risk factor; he believes it’s his animals that are at risk from spread in the wild. Because he’s enrolled in the federal monitoring program, more Americans are willing to buy his products. If chronic wasting disease were to be found within 80 kilometres of his farm, restrictions on importing cervids could mean the end of his business.
“It’s what we lose sleep over,” says Farmer, who is also vice president of the Manitoba Elk Growers Association “We spend, [on] our farm alone, probably over one million dollars on biosecurity.”

Farmer says he’s spent the better part of the last decade urging Manitoba to crack down on the mule deer population, as they seemed high risk for transmission.
He’s also been urging the government to co-ordinate with cattle farmers to fence off hay fields and other sources of deer-attracting food — like the double 12-foot fences that protect his farm.
Containing “artificial points of host concentration” was the number one recommendation in a 2018 report from the Western Association of Fish and Wildlife Agencies on chronic wasting disease. Davis says he’s now working with agriculture to increase awareness about the risks posed by leaky grain bins and exposed hay fields, but Farmer worries it’s all “too little too late.”
“We’re just hoping with what they’re doing now that it’ll slow the spread,” he says.
Impacts of uncontrolled disease spread could be dire
Calling from the road as he drives towards Piikani First Nation in southern Alberta, Alliance for Public Wildlife director Darrel Rowledge isn’t in the mood to mince words. “If we ever end up with a pandemic of this particular prion disease that manifests in people as it does in deer, it would be horrendous,” he says.
According to a report Rowledge co-authored in 2017, research has shown the disease makes deer 4.5 times more likely to die than healthy deer, and contributed to an annual population decline of 19 per cent in a monitored herd in Wyoming. Some models have suggested the disease, unchecked, can lead to localized extinction as it spreads among cervid family groups.
“If it’s extinction for deer,” Rowledge asks, “What the hell does this mean [for people]?”

Debate rages over the true risks the disease might pose to people: some experts argue prion diseases like scrapie have persisted in wildlife for centuries without human infection, while others point to outbreaks of the human version of mad cow disease as cause for concern. Recent testing on mice, squirrels and monkeys have suggested chronic wasting disease could one day manifest in humans, but so far no cases have been found.
Health Canada has not made any outright statements about the risks of a human strain of chronic wasting disease, but has said infected animals “should not be consumed.” But with a lack of regulation and limited education about the disease — not to mention how long it takes to get test results — the Alliance has estimated between 7,000 and 15,000 diseased cervids are eaten every year across North America. In 2019, the Canadian Food Inspection Agency set off alarm bells after warning advocacy group BloodWatch that elk meat from 21 infected herds had entered the food chain since 2014.
From the helm of the Alliance — a group of scientists and researchers developing and promoting policy to protect North American wildlife — Rowledge has written letters, research papers, a book and even a film to try and convince provincial and federal governments that holistic, aggressive and immediate actions are “vital” to preventing a looming tragedy. Though he’s not a scientist himself, Rowledge has worked alongside experts to develop policy recommendations around chronic wasting disease.
Though it hasn’t proven infectious to people yet, the potential outcome of crossing the species barrier would be catastrophic. There are no therapeutics, no vaccines, no clear way to eradicate an infection once it starts. Unlike mad cow disease, which was passed between animals and people solely by eating infected meat, chronic wasting disease is considered far more contagious since the prions are known to transfer through bodily fluids and stick around in the environment.
Diseased cervid populations could impact food security for those who rely on deer, moose and elk for protein, Rowledge says.
In 2017, Piikani Nation chief Stanley Grier told the Assembly of First Nations chronic wasting disease “threatens irreparable harm to wildlife and to First Nations rights to hunt, fish, gather as promised under the numbered Treaties across Canada.”
There are, he said, “direct implications for reliant peoples and communities,” especially if the disease spreads to caribou.
To help mitigate the disproportionate risk to First Nations, the Assembly distributed a technical bulletin to First Nations in 2019 advising hunters — who rely on animals for food and social and ceremonial practices — about the risks of the disease. The Assembly wrote it’s committed to developing “better resources” to raise awareness of chronic wasting disease among First Nations.

Both mad cow disease and COVID-19 have shown how zoonotic diseases can devastate local and global economies. When mad cow disease was found in Alberta, the ensuing trade restrictions cost Canadian beef producers more than $5 billion. In 2021, B.C. announced plans to shut down its entire mink industry because of COVID-19 spread.
Similar effects are already being felt in jurisdictions with significant hunter economies. In 2011, Saskatchewan’s game farm industry was estimated to contribute $15 million per year to the provincial economy, but that industry is on the decline. Wisconsin has estimated chronic wasting disease contributed to revenue losses of between $45 million and $72 million per year.
Recognizing that chronic wasting disease persists in the environment, Norway has already banned the import of hay or straw from any province or state with confirmed chronic wasting disease cases.
All told, Rowledge believes chronic wasting disease presents “the most outrageous human susceptibility experiment in history.”
Manitoba hunters on board with management efforts
According to Davis, only “time will tell” whether the disease has been beaten back behind Manitoba’s borders.
The good news is that hunters seem increasingly on board with the province’s containment methods.
Life-long hunter Armin von Hacht, who lives in Winnipeg, shot five deer this year. After meticulously cleaning and separating the meat, he stored the carcasses in his freezer and sent the heads in for testing. The carcasses will stay in the freezer until his results come in.
“Chronic wasting disease … scares the bejesus out of me,” he says.

Keenly aware of the risks, von Hacht feels a responsibility to help stop the spread. He communicates with other hunters and maintains a good relationship with the department of natural resources and the farmers in his community. He says he would abstain from hunting if necessary.
“We’ve got so many diseases from all across the world now. We share everything in this world — at least the bad stuff. This is just another one of those things that we have to be concerned about going forward, just like COVID,” he says.
“If this spreads and it’s not controlled, we’re all in big trouble.”
Much like with public health measures brought in to combat COVID-19, von Hacht says, “some people are going to co-operate, some people won’t,” but the key is education, helping everyone understand their role in mitigating the spread.

It’s that sense of community cooperation that experts like Rowledge and Davis believe is necessary to underpin any government strategy.
“Everything is interconnected in the world and what impacts one will impact others,” Davis says.
If deer populations start to dwindle as a result of chronic wasting disease, he says, “that’s going to reduce the biodiversity on the landscape itself and have broad-reaching concerns.”
“People are involved in that — we’re not separated from the environment.”




